Key Takeaways:
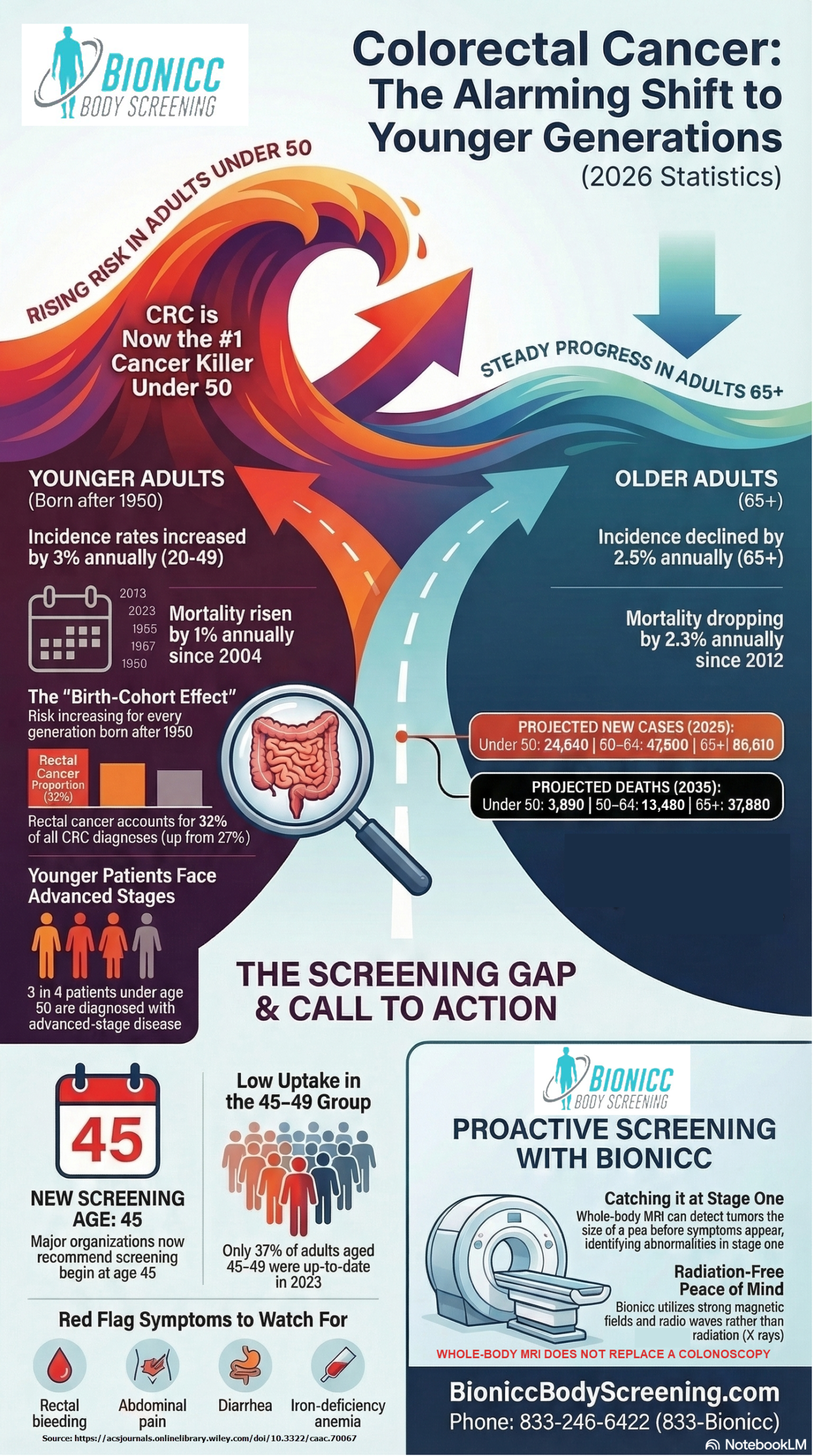
- Colorectal cancer incidence is rising by 3% annually in adults under 50, making it the leading cause of cancer death for this demographic.
- Major health organizations now strongly recommend that average-risk adults begin colorectal cancer screening at age 45 rather than age 50.
- Standard medical screenings like colonoscopies and mammograms only monitor areas where roughly 29% of cancers develop, leaving a massive 71% blind spot in the body.
- Many young adults diagnosed with advanced colorectal cancer are physically fit and show absolutely no early symptoms.
- Full body MRI scans provide a safe, radiation-free method to detect solid tumors as small as a pea across the entire body, however, they do not replace a colonoscopy and are limited for evaluation of the colon.
- Patients can secure proactive health intelligence without a doctor’s referral, gaining total control over their personal wellness.
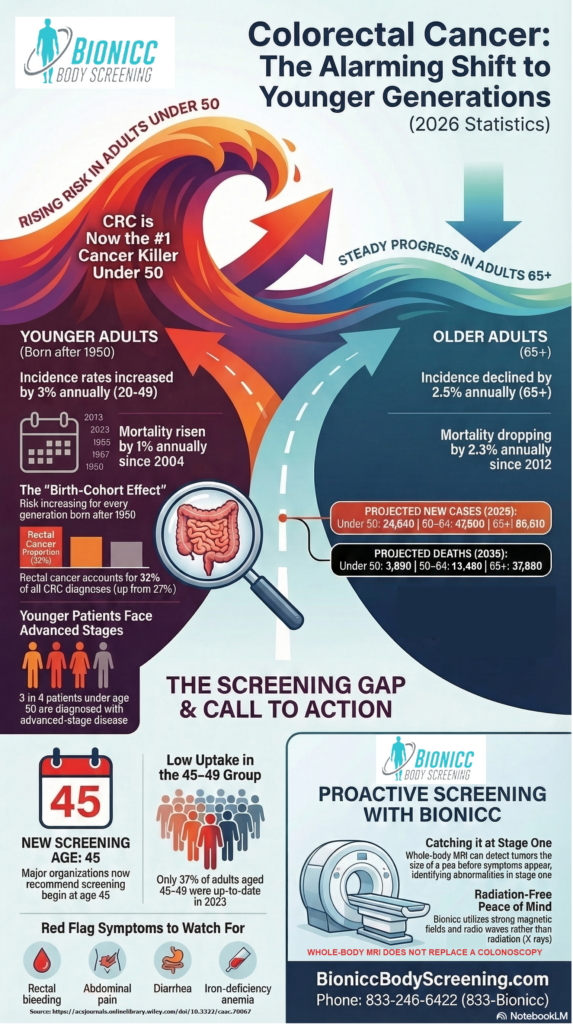
Table of Contents
The Shifting Landscape of Preventative Health in 2026
For many decades, colorectal cancer was viewed almost exclusively as a disease of old age.
Medical textbooks and public health campaigns focused entirely on senior citizens. Today, that narrative has completely collapsed. A new and deeply concerning reality has emerged in 2026 and the key to battling it is early colorectal cancer detection.
The American Cancer Society reports that colorectal cancer rates are rising sharply in younger generations. Adults in their 20s, 30s, and 40s are facing unprecedented risks. At the same time, traditional medical guidelines often leave these younger patients highly vulnerable.
Many young adults are frequently told they are simply too young for routine cancer screening. This gap in routine preventative care carries deadly consequences. When younger adults finally receive a diagnosis, the disease is very often in an advanced stage.
The tumors have usually already spread to other organs. This makes treatment much more difficult and drastically lowers survival rates. However, individuals are not powerless against this rising threat.
The rapid advancement of imaging technology is fundamentally changing how people approach their healthcare. Tools like full body MRI scans are giving individuals the power to look clearly inside their own bodies.
These preventative scans offer profound peace of mind; however, it is critical to note that a full body MRI does not replace a colonoscopy and is limited in the evaluation of the colon.
They are designed to catch hidden abnormalities while they are still small and highly treatable throughout the major organs.
This comprehensive report explores the shifting statistics of colorectal cancer. It details the limitations of traditional screening methods and highlights the life-saving benefits of proactive full body MRI technology.
What is early-onset colorectal cancer?
Early-onset colorectal cancer refers to the diagnosis of colon or rectal cancer in individuals under the age of 50. Driven by environmental factors, diet, and genetics, it frequently presents at an advanced stage because younger adults are often excluded from routine screening protocols until age 45.
The Stark Reality of 2026 Colorectal Cancer Statistics
To truly understand this health crisis, one must examine the latest data.
In 2026, an estimated 158,850 new cases of colorectal cancer will be diagnosed in the United States. This massive figure equals roughly 440 new medical diagnoses every single day.
Sadly, the disease remains highly lethal when it is caught late.
An estimated 55,230 people will die from colorectal cancer in 2026. It currently stands as the second most common cause of cancer-related death in the entire country.
Historically, the medical community was making excellent progress against this disease. The overall incidence rate actually declined by 0.9% annually from 2013 to 2022. However, this progress was driven almost entirely by improvements among older adults.
In adults aged 65 and older, incidence rates dropped by an impressive 2.5% per year. Widespread Medicare coverage for preventative colonoscopies helped drive this success for older generations.
When precancerous polyps are found and removed during a routine colonoscopy, the cancer is prevented entirely. But while the oldest adults are seeing continuous improvements, younger generations are facing a steep and sudden crisis.
A Breakdown of the Expected 2026 Cancer Burden
The data reveals exactly how the disease is distributed across different age groups. The table below breaks down the estimated 2026 colorectal cancer burden by age group.
| Age Group (Years) | Estimated New Cases | Percentage of Total Cases | Estimated Deaths | Percentage of Total Deaths |
|---|---|---|---|---|
| Birth to 49 | 24,640 | 16% | 3,890 | 7% |
| 50 to 64 | 47,600 | 30% | 13,480 | 24% |
| 65 and Older | 86,610 | 55% | 37,860 | 69% |
| All Ages | 158,850 | 100% | 55,230 | 100% |
Nearly half of all new diagnoses (45%) now occur in individuals under the age of 65. This is a massive demographic shift from 1995. Back then, only 27% of cases occurred in this younger age group.
The patient population is rapidly shifting younger and younger. This dramatic shift challenges everything modern doctors thought they knew about the disease.
The Generational Threat: Understanding the Birth-Cohort Effect
Medical researchers refer to this alarming phenomenon as a “birth-cohort effect.” This means a person’s risk of getting the disease is closely tied to the specific decade they were born.
Incidence is not just increasing for young people overall. It is increasing specifically for every single generation born after the year 1950. As these specific generations age, they carry this higher underlying risk with them into their later years.
Experts warn that as these younger cohorts reach their 60s and 70s, the overall cancer burden will swell dramatically. It is described as a tsunami of disease moving through time. This makes early detection more critical now than ever before in modern history.
For adults aged 20 to 49, incidence rates have increased by a shocking 3% every year since 2013. Because of this relentless upward trend, colorectal cancer is now the leading cause of cancer-related death in adults under 50.
Even adults aged 50 to 64 are seeing a noticeable uptick in disease. Incidence in this middle-aged group is rising by 0.4% annually. This completely reverses years of previous historical declines.
The death rate for young adults is also climbing steadily. Mortality for those under 50 has increased by 1% annually since 2004. This tells the medical community that the disease is not just becoming more common. It is remaining deadly for those who catch it too late.
Anatomical Shifts: The Dangerous Rise of Rectal Cancer
The disease is also fundamentally changing where it appears inside the body. Colorectal cancer can occur in the proximal colon (the right side), the distal colon (the left side), or the rectum.
Historically, right-sided tumors were the most common variation found in older adults.
However, the modern surge in young adults is dominated almost entirely by tumors in the distal colon and the rectum.
From 1998 to 2022, the incidence of rectal cancer nearly doubled in adults aged 20 to 49. Today, rectal cancer accounts for 32% of all colorectal cancers across all age groups.
This is a significant increase from just 27% in the mid-2000s.
Rectal tumors often present highly unique challenges for both patients and surgeons. Treating them can have severe and lasting impacts on a patient’s daily quality of life.
Surgeries in this highly sensitive area can negatively affect sexual function, fertility, and bowel control. Catching these specific rectal tumors early is absolutely vital to preserving normal bodily functions.
Colorectal Cancer Statistics in Michigan
Access to preventative care varies wildly depending on where a person lives. The American Cancer Society tracks these geographic disparities very closely.
State-level patterns reveal that the colorectal cancer burden is generally highest in Appalachia, the South, and parts of the Midwest. Conversely, rates are typically lowest in the Northeast and the Western regions of the United States.
These stark differences reflect wide variations in the local prevalence of known risk factors. States with higher rates of smoking and excess body weight consistently report higher cancer numbers.
In Michigan, the colorectal cancer incidence rate is 34.3 per 100,000 for White individuals and 39.7 per 100,000 for Black individuals. The overall mortality rate in the state sits at 13.5 per 100,000.
While Michigan boasts a relatively high colorectal screening rate of 72% for adults over 45, significant health gaps remain. Education plays a major role in whether a person gets screened.
In Michigan, screening compliance is 80.2% for college graduates. However, that number plummets to just 60.1% for individuals with less than a high school diploma.
These statistics prove that much more community outreach is desperately needed. Innovative facilities like Bionicc Body Screening help bridge this gap. They offer direct-to-consumer healthcare that bypasses traditional bureaucratic hurdles.
Residents across Metro Detroit and beyond can access top-tier imaging without navigating complex insurance approvals or restrictive referral networks.
Decoding the Root Causes of the Epidemic
Why exactly is colorectal cancer skyrocketing in younger generations? Scientists have not found one single, definitive smoking gun.
Instead, leading researchers point to a perfect storm of environmental and lifestyle factors. Over the last 50 years, the standard American diet has changed drastically.
Ultra-processed foods have completely flooded the commercial market. These highly engineered foods are packed with artificial chemicals, preservatives, and refined sugars.
At the exact same time, daily physical activity has plummeted across the population. Sedentary lifestyles and rising obesity rates are closely and undeniably linked to colon cancer risk. High consumption of red meat and heavy daily alcohol use also play major contributing roles.
The Gut Microbiome and Chronic Inflammation
Medical researchers are now deeply focused on the human gut microbiome. This is the massive, complex ecosystem of bacteria naturally living in the human digestive tract.
When a person’s diet is poor, these bacteria become severely unbalanced. This dangerous condition is known medically as dysbiosis.
Dysbiosis creates a state of chronic, low-grade inflammation along the delicate gut lining. Over many years, this constant inflammation can damage healthy cells. This cellular damage eventually triggers the rapid growth of cancerous tumors.
Antibiotic overuse during childhood and continuous exposure to environmental microplastics are also being studied as potential culprits. The exact root cause remains a complex mystery. This uncertainty makes proactive, imaging-based screening the only truly reliable defense.
Emerging Research: Can GLP-1 Agonists Lower Risk?
Interestingly, some modern weight-loss medications might offer unexpected preventative benefits. Recent medical studies have looked closely at GLP-1 receptor agonists, such as Ozempic.
These popular drugs are primarily prescribed to treat type 2 diabetes and clinical obesity. Research published in the prestigious JAMA Network Open analyzed the medical records of 1.6 million patients.
The extensive study found that patients actively using GLP-1 medications had a significantly lower risk of developing colorectal cancer. While much more clinical research is needed, this strongly suggests that treating underlying obesity and metabolic issues can directly lower a person’s cancer risk.
The Tragic “Symptom Trap”
One of the absolute biggest dangers of early-onset cancer is what medical experts call the “symptom trap”. People mistakenly believe that if they feel healthy, they simply do not have cancer.
Colorectal cancer is famously known as a silent killer. In its earliest and most treatable stages, it produces absolutely no physical symptoms. Tumors can grow slowly inside the bowel for years without causing a single noticeable ache or pain.
By the time symptoms finally appear, the cancer has usually grown large enough to bleed heavily or physically block the intestines. Common symptoms include severe abdominal pain, unexplained weight loss, extreme daily fatigue, and visible blood in the stool.
If a patient waits until they experience these glaring red flags, the cancer is frequently already at an advanced stage. Late-stage treatment requires harsh systemic chemotherapy, highly invasive surgeries, and punishing radiation.
The Illusion of Fitness: The James Van Der Beek Case
The profound danger of ignoring preventative screenings was tragically highlighted by the case of famous actor James Van Der Beek.
Known widely for his leading television roles, Van Der Beek was diagnosed with stage 3 colorectal cancer at the young age of 48.
He sadly passed away in early 2026, leaving behind a young family. Van Der Beek’s story deeply shocked the American public. He was not an older, sedentary man with poor health habits.
He was in his 40s and in peak cardiovascular shape. He ate a healthy, conscious diet and exercised vigorously and regularly.
When he first noticed mildly irregular bowel movements, he assumed it was just his daily coffee intake. By the time he finally received a diagnostic colonoscopy, the cancer had already reached a deadly stage 3.
“I was in amazing cardiovascular shape, and I had stage 3 cancer, and I had no idea,” he told the public shortly before his passing. His tragic story proves definitively that youth and physical fitness cannot replace the absolute need for proper medical screening.
The Evolution of Medical Screening Guidelines
In response to the mounting public health crisis, the medical establishment finally took decisive action. In 2018, the American Cancer Society officially lowered the recommended screening age for average-risk adults.
The guideline was dropped from age 50 down to age 45. The U.S. Preventive Services Task Force formally followed suit in 2021.
Now, all adults in the United States are strongly urged to begin routine colorectal cancer screening at age 45. If a patient has a known family history of the disease, or genetic markers like Lynch syndrome, they should start screening even earlier in life.
Unfortunately, the general public has been dangerously slow to adopt these new life-saving rules. Since the recommended age was lowered, fewer than 1 in 4 adults aged 45 to 49 have actually completed a screening.
Overall, more than 1 in 3 adults over the age of 45 remain totally unscreened and unprotected. This massive gap in preventative care leads directly to thousands of preventable deaths every single year.
Evaluating Traditional Screening Methods
For decades, patients have relied on a few standard medical methods to screen for colorectal cancer. Each specific method has its own distinct strengths and serious limitations.
Colonoscopy: The Gold Standard
A colonoscopy involves inserting a long, flexible tube with a camera into the rectum to visually inspect the entire colon. It is highly accurate and allows doctors to immediately remove precancerous polyps on the spot.
However, the procedure is highly invasive. Patients must undergo a miserable, day-long bowel preparation process involving strong, unpleasant laxatives. They also require medical sedation and a driver to take them home afterward.
There is also a small but real risk of serious medical complications, like bowel perforation or severe internal bleeding. Because of these highly unappealing factors, many patients simply refuse to get one.
Stool-Based Tests
To improve patient compliance, non-invasive stool tests were rapidly developed. The Fecal Immunochemical Test (FIT) looks closely for hidden microscopic blood in the stool.
More advanced stool DNA tests, like Cologuard, look for both hidden blood and altered DNA shed by shedding cancer cells. These tests are remarkably easy to do in the privacy of your own home.
However, they are far from perfect. They can easily miss flat lesions or smaller, developing polyps. Furthermore, if a stool test comes back positive, the patient must still immediately undergo a full colonoscopy to find the root cause.
Sadly, a recent clinical study showed that only 53% of patients who get a positive stool test actually follow up with a colonoscopy within a year. This failure completely erodes the entire benefit of the initial home screening.
The 71% Blind Spot in Routine Healthcare
While colonoscopies and mammograms are incredibly important tools, they highlight a major, systemic flaw in modern healthcare. These traditional tests only look at very specific, highly isolated body parts.
Routine cancer screenings covered by typical health insurance plans only detect about 29% of incident cancers. This is a truly shocking statistic that most patients do not know.
It means that 71% of all cancers occur in areas of the body that are never routinely checked by standard doctors. Deadly cancers forming in the pancreas, liver, brain, kidneys, and chest are left entirely unmonitored.
A patient could get a perfect, clean score on their colonoscopy and their mammogram, while a deadly tumor grows silently inside their kidney. To truly protect long-term health, individuals need a tool that looks at the entire biological picture.
How does a full-body MRI detect cancer?
A full-body MRI detects cancer by utilizing powerful magnetic fields and radio waves to generate high-resolution images of internal organs and soft tissues. It identifies tumors, cysts, and structural abnormalities as small as a pea without exposing the patient to harmful ionizing radiation.
Magnetic Resonance Imaging (MRI) is a revolutionary tool in modern preventative medicine. Unlike traditional X-rays or CT scans, MRI does not use any ionizing radiation.
Radiation from repeated CT scans can eventually damage DNA and actually increase a person’s cancer risk over a lifetime if overused. Because an MRI uses entirely safe magnetic fields, there is zero cumulative radiation risk.
A patient can safely undergo an MRI every single year to closely monitor their health without fear of radiation exposure.
Unmatched Imaging Precision and Accuracy
MRI technology offers incredible, unmatched soft-tissue contrast. It allows highly trained radiologists to clearly distinguish between healthy tissue, benign fluid-filled cysts, and malignant solid tumors.
When cancer is found at stage one, long before it has a chance to spread, the 5-year survival rate exceeds 90%. Advanced MRI technology makes this critical level of early detection a daily reality.
Establishing a Health Baseline with Medicine 3.0
The traditional American healthcare system is built entirely on reactive medicine. You get sick, you show visible symptoms, and then the doctor tries desperately to fix you. By then, it is often a massive, uphill battle.
“Medicine 3.0” is a rapidly growing new philosophy. It focuses entirely on proactive, data-driven disease prevention. The ultimate goal is to optimize human health and catch microscopic biological changes years before they become deadly emergencies.
Investing in a full body MRI while you feel perfectly healthy establishes a high-definition “internal dashboard”. This creates a highly precise medical baseline tailored uniquely to you.
If you receive a follow-up scan five years from now and a single lymph node is slightly enlarged, doctors do not have to guess what happened. They can simply look back at your original baseline scan to see exactly when the subtle change occurred.
This shifts your healthcare from a series of stressful emergency repairs to a strategic, lifelong maintenance plan.
Bionicc Body Screening: A Mission Rooted in Personal Experience
For many years, full body MRI scans were completely inaccessible to the general public. They were reserved only for the ultra-wealthy or elite professional athletes. Today, dedicated imaging clinics are making this life-saving technology available to everyday people.
Bionicc Body Screening’s About Us page reveals the deeply personal and moving story behind Michigan’s premier preventative imaging center. Bionicc Body Screening in Southfield, Michigan, was founded by the late Dr. Warren Ringold.
Dr. Ringold was a dedicated physician who felt completely healthy until he suddenly experienced a mild shortness of breath. A subsequent trip to the hospital revealed the unthinkable. He had stage 4 cancer.
He endured the brutal, ravaging treatments of late-stage disease. Though he survived the initial agonizing bout, the cancer later returned aggressively as a brain tumor.
In his final days, Dr. Ringold was fueled by a deep passion to spare others from this terrifying journey. He established Bionicc Body Screening to provide the proactive, early-detection imaging he desperately wished he had access to earlier in life.
Today, his son Ryan Ringold carries on this vital, life-saving mission. As the Managing Director and Patient Advocate, Ryan ensures that everyday people can access the exact tools needed to detect the 71% of cancers missed by routine medical checks.
Read the article Prenuvo Scan Alternative in Michigan to see how Bionicc Body Screening compares with Prenuvo.
Demystifying the Patient Experience
Many people avoid MRI scans because they fear tight spaces, loud noises, or confusing medical jargon. Bionicc Body Screening has completely streamlined the entire process. It is designed to be comfortable, fast, and empowering.
Patients do not need a doctor’s referral or permission to book an appointment. They can simply call 1-833-BIONICC (833-246-6422) or book directly online from their own home.
On the day of the scan, patients check in at the welcoming Southfield full body MRI center and are escorted to a private, comfortable room. If their clothing contains any metal, they are provided with soft hospital pants and a gown.
The machine itself is a state-of-the-art Siemens Magnetom Aera 1.5T. This is a specialized “wide-bore” MRI machine. It offers significantly more space and comfort, especially for patients who experience claustrophobia.
Patients are given a choice of music to listen to while they relax inside the machine. The actual scanning process takes only about 70 minutes. Including check-in and check-out, the entire visit lasts roughly 2 hours. It is a fast, painless process that yields decades of priceless health intelligence.
A Comprehensive Look Inside: Regions Covered by the Scan
When a patient books a scan at Bionicc Body Screening, they receive an exhaustive, meticulous evaluation of their internal anatomy. The MRI scans the body from the very top of the head all the way down through the pelvis.
The comprehensive full body screening includes deep evaluations of multiple critical systems.
Head and Neck Screening
The scan meticulously evaluates the brain for dangerous aneurysms, tumors, signs of multiple sclerosis, and evidence of past strokes. It also checks the sinuses, thyroid gland, esophagus, and cervical lymph nodes for early abnormalities.
Torso and Abdomen
The chest, abdomen, and pelvis are thoroughly imaged. This includes deep looks at the liver, gallbladder, kidneys, spleen, and pancreas. It can reliably diagnose fatty liver disease and check for silent, deadly aortic aneurysms.
Urinary and Reproductive Systems
The bladder and kidneys are checked for masses or blockages. For women, it detects early lesions in the uterus and ovaries. For men, it screens the prostate for dangerous enlargement or tumors.
Digestive Review
The scan looks for massive inflammation or large masses in the digestive tract. While it does not replace a colonoscopy and cannot detect polyps, it can catch tumors constricting the bowel that are 1.5 cm or larger.
Musculoskeletal System
The entire spine (cervical, thoracic, and lumbar) is checked for herniated discs and hidden fractures. The hips and shoulders are evaluated for severe arthritis or painful inflammation.
Every single scan is read by a Michigan-licensed, board-certified radiologist with over 25 years of diagnostic experience. Patients receive a printed report, a DVD of their images, and a personal follow-up call from the medical team to discuss the results in plain English.
Analyzing the Financial Investment in Your Health
Because full body MRIs are elective, preventative procedures, they are generally not covered by traditional health insurance plans. Patients must pay out of pocket for this premium service.
However, when compared directly to the catastrophic financial toll of a late-stage cancer diagnosis, the cost of a preventative scan is a minimal, highly logical investment.
At Bionicc Body Screening, patients can choose from three distinct screening packages: Head and Neck, Torso, or Full Body.
Bionicc Body Screening pricing ranges from $1,299 to $2,950. To make this vital technology highly accessible, Bionicc offers 0% interest financing for up to 12 months for qualified individuals.
Flexible payment plans can start as low as $168 a month. Families who wish to protect multiple members can also take advantage of generous couples discounts. Booking two Full Body MRI screenings together saves a total of $700.
Individuals insure their homes, their cars, and their cell phones without a second thought. A person’s health is their absolute most valuable asset. Investing in a baseline scan ensures you remain healthy and physically present for the people who depend on you the most.
Overcoming Psychological Barriers to Screening
If medical screening definitively saves lives, why do so many people avoid it? The answers are deeply rooted in human psychology.
The Colorectal Cancer Alliance recently conducted a massive State of Screening study. They found that ongoing gaps in awareness, concerns about financial cost, and intense fear of physical discomfort are massive societal hurdles.
Many people are simply terrified of finding out they are sick. This primal fear causes them to bury their heads in the sand. But medical ignorance does not stop a disease. It only allows the disease to grow in the dark, unchallenged.
Advanced imaging completely removes the physical discomfort from the screening equation. There is no invasive medical scope. There is no fasting or painful bowel preparation required.
An MRI is completely non-invasive. You simply lie still, relax, and let the powerful magnets do all the work. By removing the fear of the physical procedure, Bionicc Body Screening makes it easy to embrace preventative health.
Finding a small medical issue early is not a death sentence. It is a profound, life-saving victory. It means you caught the problem in time to fix it easily and move on with your life.
Empowering Patients Through Action
The dramatic, statistical rise in early-onset cancer is undoubtedly scary. But the data clearly shows that society has the technological tools to fight back.
People no longer have to rely solely on outdated, reactive medicine. Individuals do not have to wait for the deadly “symptom trap” to spring shut.
By understanding the severe risks of modern diets, acknowledging the rapidly changing cancer statistics, and utilizing advanced MRI technology, individuals can rewrite their own health narrative.
Knowledge is ultimate power. A full body MRI provides the ultimate, high-definition map of your internal health. It shines a bright light on the 71% blind spot that traditional medicine routinely ignores.
It gives you the actionable intelligence needed to make highly informed decisions about your future. Do not wait for symptoms to appear. Take control of your health today.
Conclusion: Securing Your Future Health
The 2026 colorectal cancer statistics deliver a clear, undeniable, and urgent message. While older generations are benefiting greatly from decades of targeted screening, younger adults are facing a silent and rapidly growing epidemic.
The shifting anatomical locations of tumors, the rise of the generational birth-cohort effect, and the tragedy of late-stage diagnoses in seemingly healthy individuals all point to an outdated healthcare model.
To effectively combat this, the medical community must expand its vision. Traditional screening tools like colonoscopies and stool tests remain vital, but they are no longer enough on their own. They simply do not cover enough of the human body.
Full body MRI technology represents the true future of preventative oncology. By providing safe, radiation-free, comprehensive imaging, it allows patients to establish a baseline of health and catch abnormalities at their most treatable stages.
Facilities like Bionicc Body Screening in Southfield, MI are proudly leading this proactive charge. They are democratizing access to elite medical imaging. They are honoring the legacy of those lost to late-stage disease, and empowering the public to adopt a Medicine 3.0 mindset.
You possess the power to actively protect your longevity. An investment in a simple, hour-long scan today can successfully secure decades of healthy, vibrant living tomorrow.
Contact Bionicc Body Screening today to book your full body MRI. To learn more, read the answers to the most frequently asked questions about full body MRI in Michigan.
Frequently Asked Questions and Answers
If I’m physically fit and have no symptoms, do I really need to be screened?
Yes. Colorectal cancer is often a “silent killer,” meaning it produces no symptoms in its earliest, most treatable stages. High-profile cases, such as actor James Van Der Beek, demonstrate that even individuals in peak physical condition can be diagnosed with advanced-stage cancer. Proactive screening is the only way to detect abnormalities before they become symptomatic.
At what age should I start colorectal cancer screening?
Current guidelines from the American Cancer Society and the U.S. Preventive Services Task Force recommend that average-risk adults begin regular screening at age 45. However, if you have a family history of colorectal cancer or certain genetic markers, you should consult with a professional about starting even earlier.
Does a full body MRI replace the need for a colonoscopy?
No. While a full body MRI is an incredible tool for detecting solid tumors as small as a pea throughout the major organs, it is limited for colon evaluation. It can detect larger masses (typically 1.5 cm or larger), but it cannot detect the small precancerous polyps that a colonoscopy can identify and remove. The two technologies should be viewed as complementary.
Why is colorectal cancer rising so quickly in adults under 50?
While there is no single “smoking gun,” researchers point to a “perfect storm” of factors. This includes the prevalence of ultra-processed foods, sedentary lifestyles, and environmental factors that disrupt the gut microbiome. This “birth-cohort effect” means every generation born after 1950 is at a higher risk than the one preceding it.
What makes Bionicc Body Screening different from traditional medical check-ups?
Traditional screenings (like mammograms or colonoscopies) only monitor areas where roughly 29% of cancers occur, leaving a 71% blind spot. Bionicc Body Screening uses advanced, radiation-free MRI technology to scan from the head to the pelvis, providing a comprehensive “baseline” of your health and detecting issues in organs that are not routinely checked by standard insurance-based medicine.
Author: Ryan Ringold is the Managing Director and Patient Advocate at Bionicc Body Screening. Continuing the mission of his father, Dr. Warren Ringold, Ryan is dedicated to providing Metro Detroit with direct, referral-free access to gold-standard preventative imaging. By simplifying complex medical data into actionable insights, he empowers individuals to take ownership of their health through early detection.
All content is fact-checked by the Bionicc Clinical Team to ensure medical accuracy. | Published: March 20, 2026